Diagnosing adult asthma
Understanding the professional guideline
Content Table
Introduction
Who is this document for and what is it about?
This document explains the recommendations in the European Respiratory Society (ERS) clinical guidelines for the diagnosis of asthma in adults (all people aged over 18 years and over). It is aimed at people with suspected asthma, or their carers.
What are clinical practice guidelines?
Clinical guidelines are produced after a scientific process used to gather and evaluate the latest evidence in the field. Guidelines also consider the opinions of leading experts and the priorities of patients and carers who have experience of a condition. Clinical guidelines are aimed at healthcare professionals. They use them as a ‘best practice’ document in how to diagnose, manage and treat specific conditions.
What does this document include?
This document summarises the key points from the clinical guidelines. It explains them in a way that is more easily understood by people who do not work in a medical field. It will cover what asthma is and how it is diagnosed. By providing this information in an accessible way, this document aims to help people who are being tested for asthma understand more about the diagnosis process and feel informed when making decisions about care.
What is adult asthma?
Asthma is a disease that includes the symptoms of wheeze, cough and breathing difficulty. These symptoms are caused by issues in the airways that cause problems with breathing:
- Airway obstruction – when the airways are blocked from swelling or extra mucus
- Airway inflammation – when the airways are irritated causing swelling and narrowing
- Bronchial hyper-responsiveness – when the airways are overly sensitive and easily react to an irritant such as smoke, cold air or exercise. When they react, they get smaller, making breathing difficult.
Asthma can vary between people and often not all of the above symptoms happen in everyone. Symptoms can also come and go over time.
Adult asthma refers to asthma that affects people aged over 18. For children aged between 5 and 18, there are separate guidelines that are used for diagnosis.
How should adult asthma be diagnosed?
Spriometry testing
A spirometry test involves blowing into a device called a spirometer. During the test, a person is asked to breathe out as much air as they can, as hard as they can. The spirometer then measures two things: how much air can be blown out in total and how much air is blown out in the first second of the test. Both these measurements are compared to a chart to look at what is normal for that person based on their sex and age. More information on understanding the results from a spirometry test can be found on the ELF website: https://europeanlung.org/en/information-hub/factsheets/testing-your-lungs-spirometry/
Spriometry tests should be the first test that is performed when a person has suspected asthma. If the results suggest a person has asthma, the next step would be bronchodilator reversibility (BDR) testing (described below) to confirm this. If the results are normal, but a person’s symptoms still suggest asthma, further tests outlined below can be used to confirm or rule out asthma.
Bronchodilator reversibility (BDR) testing
If the spirometry test suggests a person has asthma, BDR testing should be the next step to confirm this. BDR testing involves taking a small amount of asthma medicine, known as reliever medicine, to help open up the airways. Reliever medicine is used for quick relief when symptoms appear. It works by relaxing the airways to make breathing easier.
After the medicine is taken, a spirometry test is performed again 10-15 min later to see if there is a change in the airways. If a person is able to breathe better this time, it shows the medicine has worked and stopped the airways from becoming narrow. It is therefore likely this person has asthma.
If both spirometry and the BDR test suggest a person has asthma, then these results can confirm a diagnosis.
Fractional exhaled nitric oxide (FeNO) testing
FeNO testing involves breathing into a machine that measures what someone breathes out. It looks at a part of a breath called nitric oxide. A high level of nitric oxide suggests there is swelling (inflammation) in the lungs. However, swelling that is not linked to asthma can also happen in the airways. For example, this can happen when a person has allergic rhinitis or eczema, but not asthma.
For these reasons, the results of this test should not be used on their own to confirm or rule out a diagnosis of asthma. Instead, the results should be used alongside the two tests above and looking at a person’s symptoms. If all these things point to asthma, then a diagnosis can be given.
Peak expiratory flow rate (PEFR) – peak flow testing
Known as a peak flow test, this looks at how fast a person can breathe out. The test uses a small hand-held device and can be done at a doctor’s surgery or at home. Sometimes, healthcare professionals will ask a person to keep a diary of their peak flow measurements at home over a few weeks.
This does not provide immediate results in the same way that spirometry, BDR and FeNO testing do, as outlined above. If no other form of testing is available, then it could be a useful measurement. It can also be a helpful way of looking at what causes a person’s asthma. By keeping measurements over a period of time, it is possible to look at when symptoms are worse and what was happening to cause it. For example, if someone’s asthma is linked to where they work.
Bronchial challenge
A bronchial challenge test involves irritating the airways to cause obstruction and lower a person’s breathing rate. This allows a doctor to watch how a person’s airways contract in response to a particular substance or to exercise. It also allows them to check whether someone’s asthma symptoms can be reproduced during the challenge and how they may improve with asthma medicine.
The test involves either breathing in a particular substance (known as a direct bronchial challenge test) or taking part in exercise (known as an indirect bronchial challenge test).
People with asthma will experience swelling in the airways much sooner than a person with healthy lungs. This test is done in very controlled conditions. An asthma specialist is always on hand to monitor and treat any symptoms. Reliever medication is given after the test to open up the airways again.
These tests are carried out in hospital or specialist centres but are not available everywhere. These tests could be used as an option to diagnose asthma if spirometry and BDR testing are not able to confirm or rule it out. Some people find the tests uncomfortable and they should only be carried out after a discussion with a healthcare provider.
The path to diagnosis
This diagram illustrates the suggested path someone might take before they confirm they have asthma:
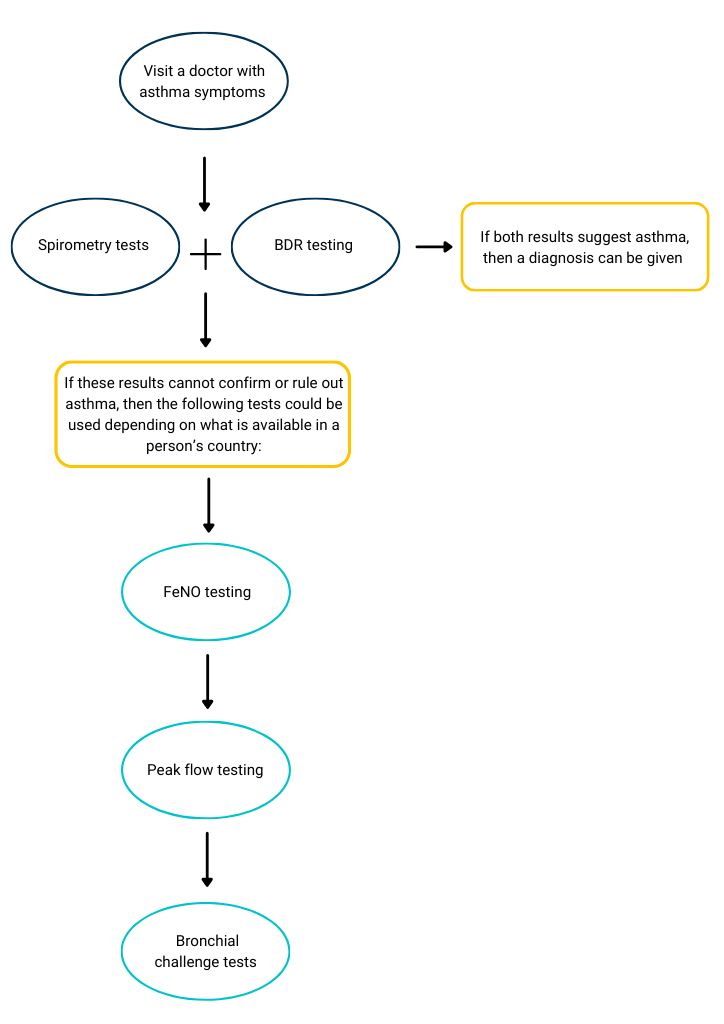
Other tests
Blood tests
Blood tests, where a small sample of blood is taken from the arm or hand, can help to understand someone’s asthma symptoms. Blood tests can help check for signs of inflammation and allergy in the body. They are commonly used to understand whether someone is allergic to a particular allergen, such as house dust mites or pollen.
They should not be used to diagnose asthma. Instead, these tests can be useful in managing asthma and understand what causes a person’s symptoms, once a diagnosis has been given.
Further reading
This guideline was produced by the European Respiratory Society and the European Lung Foundation. You can find out more about these organisations and access the full professional guideline using the links below:
Full clinical guideline – published in February 2022: https://doi.org/10.1183/13993003.01585-2021
Further resources for patients and carers:
Testing your lungs: spirometry (factsheet) https://europeanlung.org/en/information-hub/factsheets/testing-your-lungs-spirometry/
Adult asthma (lung conditions section) https://europeanlung.org/en/information-hub/lung-conditions/adult-asthma/
About ERS
The European Respiratory Society (ERS) is an international organisation that brings together physicians, healthcare professionals, scientists and other experts working in respiratory medicine. It is one of the leading medical organisations in the respiratory field, with a growing membership representing over 140 countries. The ERS mission is to promote lung health in order to alleviate suffering from disease and drive standards for respiratory medicine globally. Science, education and advocacy are at the core of everything it does. ERS is involved in promoting scientific research and providing access to high-quality educational resources. It also plays a key role in advocacy – raising awareness of lung disease amongst the public and politicians. www.ersnet.org
About ELF
The European Lung Foundation (ELF) was founded by ERS to bring together patients and the public with professionals. ELF produces public versions of ERS guidelines to summarise the recommendations made to healthcare professionals in Europe, in a simple format for all to understand. These documents do not contain detailed information on each condition and should be used in conjunction with other patient information and discussions with your doctor. More information on lung conditions can be found on the ELF website: www.europeanlung.org





